Making a Diagnosis
An accurate diagnosis is the cornerstone of effective treatment. Without it, even the best treatments may fail to produce results. In this blog, we’ll explore the process of making a diagnosis and why it’s more than just getting a scan.

The Three Key Components of Diagnosis
Diagnosing a musculoskeletal condition involves gathering and analyzing information from three main sources:
- Clinical History
- Clinical Examination
- (Sometimes) Further Investigations (e.g., X-ray, ultrasound, or MRI scan)
Clinical History: Listening to the Patient
The first and most crucial step is talking to and listening to the patient. Since many musculoskeletal conditions present with similar symptoms, the clinician will ask specific questions to narrow down the possible causes. Typical questions include:
- Where is the pain located, and what does it feel like (sharp, dull, burning)?
- How did the symptoms appear? Was it sudden or gradual?
- Are the symptoms constant, or do they come and go? Are they worse in the morning or at night?
- Do symptoms interfere with daily activities or sleep?
Additionally, the clinician will inquire about:
- Day-to-day activities (work, exercise, lifestyle)
- Any previous medical conditions or medications
- Past treatments or tests (e.g., previous X-rays or MRIs)
Clinical Examination: Observing and Testing
Once the clinical history is taken, the next step is a hands-on clinical examination. This includes:
- Observation and Palpation:
- Checking for visible signs such as swelling, redness, warmth, or muscle wasting
- Palpating the area to check for things such as lumps, bumps, any changes in tissue texture and to identify the location of any pain
- Functional Tests: Assessing movement, sensation, and muscle strength. This can involve:
- Passive and active range of motion tests
- Nerve tension tests (e.g., slump test)
- Strength tests (e.g., resistive tests)
- Specialized orthopedic tests (e.g., Tinel’s test, Phalen’s test, Jobe’s relocation test) –Many of these tests are named after the experts who developed them and they help in refining the diagnosis.
Further Investigations: When Are They Necessary?
While history and examination often provide enough information for a confident diagnosis, sometimes further investigations are needed. However, imaging investigations are not always the best first step, nor are they always necessary. Since investigations such as MRI can add additional costs for the patient, they are often only requested in certain circumstances. For example if:
- There is more than one possible diagnosis.
- Symptoms are unusual or atypical.
- The extent of the injury needs to be assessed to determine how best to treat it.
- An underlying condition like rheumatoid arthritis or gout is suspected (in which case blood tests may be required).
It is important to note that over-reliance on imaging can be misleading. Many people assume a scan will provide all the answers, but this isn’t always the case.
The Pitfalls of Relying Solely on Imaging
Radiological imaging can be useful, but it has limitations. Here’s why:
1. Normal Tissues Can Function Abnormally
Some conditions arise from functional issues, such as muscle imbalances or delayed muscle activation, which won’t appear on a scan but can be identified during an examination.
2. Structural Abnormalities Might Not Be Causing the Symptoms
For example an MRI scan may reveal degenerative changes or disc bulges, but these findings may not actually be the source of the pain. Many people over 40 have lumbar spine degeneration on an MRI, but most do not experience pain. It is therefore very important to correlate any abnormal findings on a scan with the patient’s actual symptoms. Put another way:
The question should alway’s be, “Do these imaging findings completely fit with what the patient is experiencing?”
3. Imaging May Provide an Incomplete Diagnosis
If multiple issues are present, a scan may only highlight one aspect, leading to incomplete treatment.
4. Chronic Pain Can Alter the Nervous System
Long-standing pain can lead to “nervous system wind-up,” where nerves become more sensitive to pain signals. This phenomenon does not show up on scans but can be diagnosed through clinical assessment.
Types of Radiology Imaging
We will now go on to take a brief look at the different types of imaging technologies and the common musculoskeletal applications of each one.

Ultrasound scan
Ultrasound scanning involves passing high frequency sound waves into the area through an ultrasound probe. These waves bounce off internal structures producing an echo which is translated into images. They can be helpful for identifying issues with soft tissues such as muscles, tendons or ligaments such as tears or areas of calcification.They can also identifying areas which are inflamed and filled with excess fluid (e.g. inflamed bursae).

X-Ray
X-ray machines emits electromagnetic x-ray beams (a form of ionising radiation) that pass through the body. Dense tissues such as bone absorb more X-rays and appear white on the resulting image, whereas x-rays pass more freely through softer tissues and these show up as various shades of gray. X-rays are helpful for identifying issues with bony structures such as fractures, deformities (such as cam or pincer deformities within a hip joint) and to assess how much joint space there is in an osteoarthritic joint.

MRI scan
Magnetic Resonance Imaging (MRI) scans use powerful magnets and radio waves together to produce lots of highly detailed images. They can often uncover structural abnormalities that other types of scans might miss. They produce very detailed images of soft tissues and can identify unhealthy areas within bone which may be missed on x-ray. They are usually the imaging of choice for identifying spinal pathology such as disc herniations or canal stenosis. Occasionally, a special type of MRI scan is requested which uses MRI alongside an injection of radio-opaque contrast dye to detect issues that might otherwise be difficult to see on an ordinary MRI scan. This special form of imaging is known as an MRI arthrogram. If for example, you have a shoulder injury and the clinician suspects that you have torn part of the cartilage within the shoulder joint (known as a SLAP lesion or labral tear) you will likely be referred for an MRI arthrogram. Since this technology uses very strong magnets, you may not be suitable for MRI if you have metal wires, devices or fragments in your body (e.g. pacemaker or defibrillator or metal shrapnell from a previous injury)
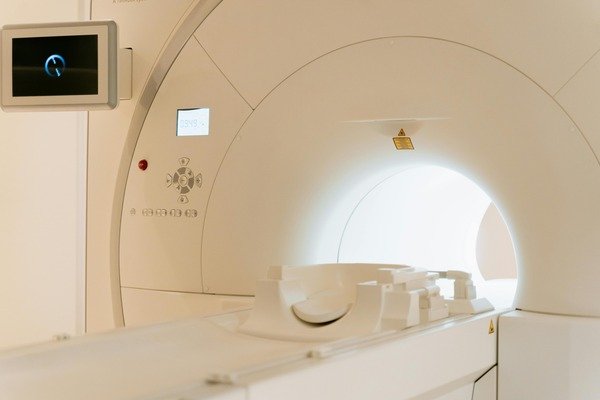
CT scan
CT scans use multiple x-ray images to build a more detailed picture, and thereby provide more 3D information than an ordinary x-ray. We don’t often request CT scans but these can on occasion be a helpful alternative where the patient needs an MRI scan but is unable to have one (for example, due to the incompatibility of a pacemaker).
Other Investigations
EMG / Nerve conduction Studies
An EMG and a nerve conduction study are tests which are typically performed at the same time. The EMG tests muscle function by measuring the electrical activity of muscles during rest (when the muscle is relaxed) and during contraction when the muscle is activated. A nerve conduction study on the other hand assesses the flow of electrical current through peripheral nerves before they reach the muscles. These tests can be useful if the clinician suspects some form of nerve damage due to injury or other underlying disease process.
Conclusion
An accurate diagnosis is about something more than just getting a scan—it requires a combination of history, examination, and sometimes targeted investigations. While imaging has its place, it should never replace a thorough clinical assessment. If you’re experiencing persistent pain or musculoskeletal issues, seek a specialist who will take the time to listen, examine, and only use further investigations when they are clinically necessary.
By understanding how diagnoses are made, you can be better informed and proactive about your health!
